| BONUS
CONTENT FROM LPN2009
Cholecystectomy:
Take a look at two options
By Bernadette R. Thomas, RN, CNOR, BSN
About 700,000 cholecystectomies
are performed each year for patients diagnosed with gallbladder
disease, making it one of the most routine surgeries performed.
The minimally invasive laparoscopic cholecystectomy is the
standard of care for most patients needing cholecystectomy.
Open surgery is an option for patients who can’t have
laparoscopic surgery.
In this article, I’ll
review gallbladder pathophysiology and your role in caring
for a patient who needs a cholecystectomy. For details on
gallbladder anatomy, see the image to the right.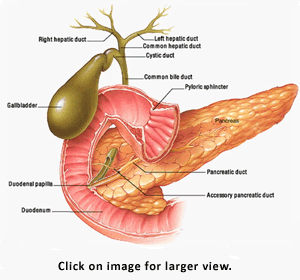
Gallbladder dysfunction
Typically, cholecystitis is caused by gallstones and is
called calculous cholecystitis. Acalculous cholecystitis,
or gallbladder inflammation without gallstones, can occur
in critically ill patients. In this article, I’ll
focus on calculous cholecystitis.
Gallstones are caused by changes
in the composition of bile, especially bile salts, phospholipids,
bilirubin, and cholesterol. When these solids are supersaturated
in the gallbladder, gallstones may form. The gallbladder
secretes mucus and proteins that promote cholesterol crystal
formation, which is the precursor for stone formation in
supersaturated bile. Impaired gallbladder motility, biliary
stasis, and changes in bile content can lead to stone formation.
For details, see Not the rolling stones.
The risk of gallstones increases
with advancing age, and women face a higher risk than men.
Other risk factors include white race, obesity, sedentary
lifestyle, alcoholism, pregnancy, rapid weight loss, oral
contraceptive use, high-fat diet, diseases of the ileum,
terminal ileum resection, parenteral nutrition, dyslipidemia,
use of cholesterol-lowering drugs, cirrhosis, hereditary
spherocytosis, and hemolytic anemia.
Diagnosing gallbladder
trouble
Signs and symptoms of cholecystitis include steady pain
in the right upper abdominal quadrant or epigastrium that
may radiate to the right scapular region or back, epigastric
or right upper abdominal quadrant tenderness, abdominal
guarding, nausea, vomiting, and fever. Abdominal pain is
similar to biliary colic but is prolonged and lasts hours
or days. (Biliary colic usually resolves gradually over
2 to 6 hours.) In about half the patients with acute cholecystitis,
pain may occur about an hour after eating a high-fat meal;
other patients may awaken from sleep with sudden pain. Another
sign of cholecystitis is a positive Murphy sign: an inspiratory
pause on right upper abdominal palpation.
To evaluate a patient for possible
cholecystitis, obtain specimens for lab tests, including
a complete blood cell (CBC) count, liver function tests,
serum amylase and lipase levels, and pregnancy test. In
a patient with cholecystitis, the CBC count typically shows
elevated white blood cell count related to inflammation;
aspartate aminotransferase, alanine aminotransferase, and
alkaline phosphate levels may also be elevated in common
bile duct obstructions.
The healthcare provider will
order imaging studies, such as an ultrasound of the right
upper quadrant (the standard imaging test). This can reveal
gallstones, gallbladder wall hickening, and pericholecystic
fluid.
In cases where an ultrasound
won’t yield clear images (for example, if the patient
is obese), the healthcare provider may order a hydroxyiminodiacetic
acid (HIDA) scan. This study can help confirm cholecystitis
by demonstrating abnormal gallbladder function.
A pear-shaped storage
tank
A distensible, pear-shaped sac located on the underside
of the right side of the liver, the gallbladder concentrates
and stores bile, which aids in fat emulsification and helps
the body absorb lipid-soluble vitamins. When food enters
the stomach, the duodenum releases cholecystokinin, the
hormone that causes the gallbladder to contract and the
sphincter of Oddi to relax, letting bile stored in the gallbladder
flow into the duodenum.
Treatment options
Most patients who need gallbladder removal are candidates
for laparoscopic cholecystectomy. Relative contraindications
to laparoscopic cholecystectomy are previous upper abdominal
surgery and some preexisting medical conditions. Laparoscopic
and open cholecystectomy are performed with the patient
under general anesthesia. Absolute contraindications to
both surgical procedures are an inability to tolerate general
anesthesia and uncorrected coagulopathy.
Laparoscopic cholecystectomy
has many benefits for patients, including a shorter hospital
stay, less pain and scarring, less trauma to tissues, a
shorter healing and recovery time, and a quick return to
normal activities (usually within 3 to 5 days). Instead
of making a 5- to 7-inch-long (12.5- to 17.5-cm-long) abdominal
incision, the surgeon makes just four small stab wounds
(see One big or four small?).
He inserts trocars at all incision sites to provide ports
of entry. This minimally invasive surgery requires a special
arrangement of equipment to provide maximum visualization.
The surgeon insufflates carbon dioxide into the abdominal
cavity through the Verres needle to establish pneumoperitoneum.
Pneumoperitoneum facilitates visualization of abdominal
structures and instrument manipulation.
The surgeon identifies the
cystic duct and artery and looks for stones in the biliary
tree with the laparoscopic instruments. After dividing the
cystic duct and artery, he dissects the gallbladder away
from the liver using a laparoscopic instrument connected
to cautery for hemostasis. After freeing the gallbladder,
he removes it through the umbilical incision. He then checks
the liver bed for bleeding and the abdomen for bile and
stones. The peritoneal cavity is decompressed of carbon
dioxide and all incisions are closed. The gallbladder and
its contents are sent to pathology for analysis.
At any time during a laparoscopic
procedure, the surgeon may convert to an open procedure
if complications arise that threaten patient safety. Possible
problems requiring open surgery include adhesions that impair
the surgeon's ability to visualize abdominal structures,
an injury to the bile duct or associated organs, gallbladder
edema, and bleeding.
Open gallbladder surgery is
much like the laparoscopic version. The surgeon examines
the biliary tree and cystic duct and handles them in the
same surgical manner. But in the open procedure, the surgeon
can use his hands to palpate for stones and can directly
examine the gallbladder before removal.
Because a patient who needs
open surgery may have major medical issues, the fragile
tissues of the inflamed gallbladder put him at greater risk
for bleeding or bile spillage. (Bile spillage also can occur
during the laparoscopic procedure because of gallbladder
inflammation or perforation with a laparoscopic instrument.)
If bile is spilled, the surgeon irrigates the abdomen with
0.9% sodium chloride solution to prevent peritonitis. He
also may place a drain in the subhepatic space.
After separating the gallbladder
from the liver bed and sending it to pathology, the surgeon
closes the muscle layers of the incision with durable sutures
that will withstand abdominal pressure. He may approximate
the skin incision line with sutures or staples, depending
on his preference.
Before the procedure
In general, preoperative care is the same regardless of
surgery type. The patient’s preoperative medical evaluation
may include blood work, a chest X-ray, and an electrocardiogram.
She should follow her healthcare provider’s directions
about taking certain medications, such as heart medications
and insulin, before surgery. She should be N.P.O. for at
least 4 hours before surgery but can usually take medication
with a sip of water.
Prepare a patient undergoing
laparoscopic surgery for postoperative shoulder and neck
pain secondary to phrenic nerve irritation from the carbon
dioxide used to insufflate the peritoneum. This minor discomfort
may last a few days, but may be relieved by changing position.
For patients having an open
cholecystectomy, review the importance of incentive spirometry,
deep breathing, and coughing after surgery to reduce the
risk of atelectasis and pneumonia. Also review the importance
of early and aggressive ambulation to help reduce the risk
of venous thromboembolism (VTE).
On the day of surgery, verify
patient identification and review the patient’s medical
history and physical, surgical history (including a personal
or family history of anesthesia problems), lab results,
limitations for positioning the patient on the OR table,
and allergies. Perform medication reconciliation, confirm
her N.P.O. status, confirm evidence of the informed consent
process, and discuss postoperative care and pain management,
including how to use a patient-controlled analgesia (PCA)
pump, if applicable.
Prophylactic antibiotics will be administered within 1 hour
prior to the surgical incision and a nasogastric tube will
be inserted for gastric decompression once the patient is
under general anesthesia.
After the procedure
Most patients who’ve had laparoscopic cholecystectomy
are discharged after 4 to 8 hours of observation. She should
be hemodynamically stable, alert and oriented, tolerating
oral fluids, and she should have voided. Her pain and nausea
should be controlled; her surgical dressings, clean, dry
and intact. A patient who’s had open surgery will
remain in the hospital for 2 to 3 days.
Postoperative care for patients
is the same for both types of surgery. Regularly assess
your patient’s level of consciousness and vital signs
and monitor her closely for signs and symptoms of bleeding.
Use a valid and reliable pain intensity rating scale to
assess her pain and provide optimal pain management. If
she has a PCA pump, review how to use it.
Check dressings for drainage
and incision sites for signs of infection. Persistent pain
unrelieved by analgesics, persistent fever over 101°
F (38° C), chills, abdominal distension, anorexia, persistent
nausea and vomiting, and jaundice may indicate bile duct
injury and should be reported immediately to the surgeon.
Place a patient who’s
had an open cholecystectomy in low Fowler’s position.
When she’s alert, encourage her to use the incentive
spirometer. Show her how to splint her incision when necessary.
After laparoscopic surgery,
position the patient in a left side-lying Sims position
to move retained pockets of carbon dioxide away from the
diaphragm and decrease discomfort.
Encourage early and aggressive
ambulation after surgery to help prevent VTE. Evaluate the
patient’s hemoglobin and hematocrit levels and notify
the healthcare provider if they’re abnormal. Follow
the American College of Chest Physicians evidence-based
clinical practice guidelines for VTE prophylaxis, depending
on level of thromboembolism risk.
The patient should start with
clear liquids and gradually advance her diet as tolerated.
She should eat a high-fiber diet and drink plenty of fluids
unless contraindicated. If she has cramping in the right
upper abdominal quadrant, advise her to reduce her fat intake.
Explain that feces will pass
through the colon faster after cholecystectomy. She may
need a bile acid binder (such as cholestyramine or colestipol)
if she develops chronic diarrhea.
Before discharge, teach your
patient to call her healthcare provider if she has excessive
or abnormal bleeding, a fever greater than 101° F, jaundice,
abdominal distension or pain, persistent cough, or shortness
of breath. Teach her about her prescribed pain medications
and how to monitor wound healing. Also teach her to monitor
her bowel habits, especially if she’s been prescribed
a bile acid binder. Tell her that bile acid binders can
cause constipation and heartburn and can interact with other
drugs, including beta-blockers, thiazide diuretics, and
warfarin. She should take medications at least 1 hour before
or 4 to 6 hours after taking the bile acid binder and should
call her healthcare provider immediately if she has any
noticeable physical changes.
Staying well
By understanding the types of cholecystectomy, you can help
your patient before, during, and after gallbladder removal.
| Not
the rolling stones
Gallstones can be of three types:
- Yellow-green stones
are the most common type of gallstone; they’re
formed from cholesterol supersaturation in bile
and are soft.
- Black stones, formed
from high concentrations of calcium bilirubinate,
carbonate, and phosphate, are small and brittle
and usually caused by hemolytic disorders such as
hereditary spherocytosis or sickle-cell disease.
- Brown stones are
formed from calcium bilirubinate and bacterial cell
bodies. These soft, mushy stones usually are secondary
to a bacterial infection that causes bile stasis.
|
| One
big or four small?
When performing a laparoscopic cholecystectomy, the
surgeon makes four half-inch-long (1.25-cm-long) incisions
as shown below:
- one at the umbilicus
for placement of the Verres needle for insufflation
of carbon dioxide gas into the abdomen. This site
is primarily used for the camera and laparoscope.
The laparoscope magnifies the visual field and projects
it onto video screens positioned at the head of
the OR table. (An emerging technique is to perform
single-port laparoscopic cholecystectomy through
an umbilical incision.)
- one at the midline
epigastric region for the dissecting laparoscopic
instrument.
- two at the upper
right quadrant for gallbladder retraction—one
at the midclavicular line and one at the anterior
axillary line.
For an open cholecystectomy,
the surgeon makes a single large incision (called
a Kocher incision) at the right subcostal space. This
incision may extend over to the xiphoid process to
expose the gallbladder better for the surgeon. |
References
Ahrendt S, Pitt H. Biliary tract. In Townsend C, et al.
(eds), Sabiston Textbook of Surgery: The Biological
Basis of Modern Surgical Practice, 17th edition. W.B.
Saunders Co., 2004.
Hirsh J, Guyatt G, Albers GW, Harrington R, Schuenemann
HJ. Antithrombotic and thrombolytic therapy, 8th edition.
ACCP guidelines. Chest, 2008;133(6 Suppl):1S-968S.
Kelley WE Jr. Single port laparoscopic surgery. http://www.laparoscopytoday.com/2008/09/single-port-lap.html.
Oddsdottir M, Hunter J. Gallbladder and the extrahepatic
biliary system. In Brunicardi F, et al. (eds), Schwartz's
Principles of Surgery, 8th edition. McGraw-Hill Co.,
Inc., 2005.
Petty R. Surgery of the liver, biliary tract, pancreas,
and spleen. In Rothrock J, et al. (eds), Alexander's
Care of the Patient in Surgery, 12th edition. Mosby,
Inc., 2003.
Sands J. Gallbladder and exocrine pancreatic problems. In
Phipps W, et al. (eds), Medical-Surgical Nursing: Health
and Illness Perspectives, 7th edition. Mosby, Inc.,
2003.
Source: Nursing2009.
February 2009.
|